What does PDPM mean for nurses?
 Daniel Johnston
Daniel Johnston 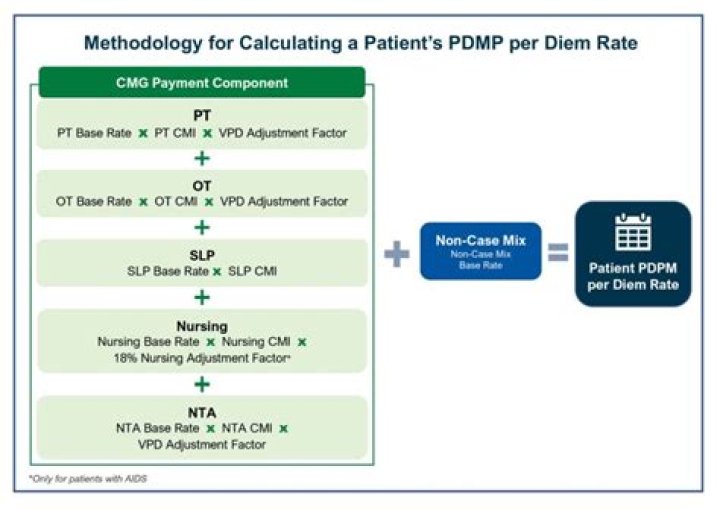
Overview. In July 2018, CMS finalized a new case-mix classification model, the Patient Driven Payment Model (PDPM), that, effective beginning October 1, 2019, will be used under the Skilled Nursing Facility (SNF) Prospective Payment System (PPS) for classifying SNF patients in a covered Part A stay.
What do I need to know about PDPM?
WHAT IS THE PATIENT DRIVEN PAYMENT MODEL (PDPM)?
- Improve payment accuracy and ensure appropriate treatment by focusing on the individual patient, rather than volume of services provided.
- Reduce administrative burden on providers.
- Improve skilled nursing facility payments without increasing total Medicare payments.
What is the definition of PDPM?
What is PDPM? Patient-Driven Payment Model. The Patient-Driven Payment Model (PDPM) is the proposed new Medicare payment rule for skilled nursing facilities. It is intended to replace the current RUG-IV system with a completely new way of calculating reimbursement.What are the 6 components of PDPM?
In the PDPM, there are five case-mix adjusted components: Physical Therapy (PT), Occupational Therapy (OT), Speech-Language Pathology (SLP), Non-Therapy Ancillary (NTA), and Nursing. Each resident is to be classified into one and only one group for each of the five case-mix adjusted components.How many types of assessments are under PDPM?
Under PDPM (effective October 1, 2019), there are 3 SNF PPS assessments: the 5-day Assessment, the Interim Payment Assessment (IPA) and the PPS Discharge Assessment. The 5- day assessment and the PPS Discharge Assessment are required.PDPM – A Comprehensive Overview
What is PDPM payment model?
The Medicare Patient-Driven Payment Model (PDPM) is a major overhaul to the current skilled nursing facility (SNF) prospective payment system (PPS). It is designed to address concerns that a payment system based on the volume of services provided creates inappropriate financial incentives.What is a 5 day PPS?
The SNF PPS establishes a Medicare-Required PPS Assessment schedule. Each required assessment supports reimbursement for a range of days of a Medicare Part A covered stay. The schedule includes assessments performed about Days 5, 14, 30, 60, and 90 of the stay.What is the function score in PDPM?
The function score for patient classification under PDPM is now calculated using data from Section GG of the MDS 3.0 (Functional Abilities and Goals) rather than Section G items. This advances CMS's goal of using standardized assessment items across payment settings. PDPM makes no changes to how Section GG is coded.What does ARD date mean?
Assessment Reference Date: The Assessment Reference Date (ARD) is the date that signifies the end of the look back period. This date is used to base responses to all MDS coding items. Ø Intent: To establish a common temporal reference point for all staff participating in the resident's assessment.What would prevent a resident from being covered under the presumption of coverage?
If the beneficiary is discharged from the hospital to a setting other than the SNF, the presumption of coverage does not apply, even if the beneficiary's SNF admission occurs within 30 days of discharge from the qualifying hospital stay.What is PDPM and PDGM?
The intent behind these administrative changes, commonly known as the Patient-Driven Payments Model (PDPM) for skilled nursing facilities (SNFs) and the Patient-Driven Groupings Model (PDGM) for home health care, is to improve the quality of patient care, promote the overall health and wellbeing of the Medicare ...What is considered an interrupted stay under PDPM?
A stay is considered interrupted whenA resident leaves the facility and returns to that same SNF no later than the third calendar day after they left. The resident remains in the facility but is no longer under Medicare A coverage, and their Medicare A coverage needs to resume within three days.
How has PDPM changed the way in which long term care facilities are reimbursed?
PDPM reimbursement, which was put into effect on October 1, 2019, shifted the emphasis from the number of visits or services and therapies provided to the particular situations and needs of patients and residents.What is the jimmo settlement?
The Jimmo Settlement means that Medicare beneficiaries should not be denied maintenance nursing or therapy when skilled personnel must provide or supervise the care for it to be safe and effective. Medicare-covered skilled services include care that improves, maintains, or slows the decline of a patient's condition.What means patient driven?
Patient-driven health care can be characterized as having an increased level of information flow, transparency, customization, collaboration and patient choice and responsibility-taking, as well as quantitative, predictive and preventive aspects.What does PDGM stand for in home health?
Overview of the HH PPS Case-Mix Model:CMS finalized a new case-mix classification model, the Patient-Driven Groupings Model (PDGM), effective January 1, 2020. The PDGM relies more heavily on clinical characteristics, and other patient information to place home health periods of care into meaningful payment categories.